The short version: Each extra drink you have per day probably takes an extra year off your life. This may or may not be true for the first 1-2 drinks per day, but it definitely is after that. If you feel like you’re drinking too much, you may want to quit; although some people succeed at drinking in moderation, people are more likely to succeed if they set out to stop drinking entirely. If you’re currently drinking more than about five drinks per day or so, you will want to take steps to avoid potentially dangerous withdrawal when you quit. Once you’ve quit, you will need to maintain your sobriety; many people find support groups or medication helpful. The support group could be Alcoholics Anonymous, but it doesn’t have to be, and there are various good secular alternatives. The best-supported medication is the anti-craving drug naltrexone. People who want to pursue moderate drinking can benefit from the Sinclair method, in which they take the naltrexone just before drinking, which breaks the link between alcohol and neural reward. You can also “tie yourself to the mast” by taking disulfiram (“Antabuse”), which makes drinking alcohol extremely unpleasant or even dangerous. Good support and medication can raise your chances, but most people won’t succeed the first time they try to quit, and should be prepared for a two-steps-forward, one-step-back process of gradually achieving better control.
The long version:
1. What’s a safe amount to drink? What are the risks of drinking more than that?
I’m going to start with a boring technical answer, and then move on to a meaningful answer later.
The boring technical answer is: experts define a “standard drink” as about the amount of alcohol in a can of beer, a glass of wine, or a shot of whiskey, usually about 12g. If you want to get fancier or more complicated than that, you can use this calculator.
CDC guidelines say that men should limit themselves to at most 14 drinks/week, and women to 7 drinks/week. USDA guidelines say 7 drinks/week regardless of gender. Other countries are more permissive; I did some of my medical training in Ireland, which allows 17 for men and 11 for women.
(Why do women get fewer drinks? Women generally weigh less, and store more of their weight as fat to provide an energy reserve for future childbearing. That means they have less lean mass for the alcohol to disperse through. Women also have lower levels of alcohol dehydrogenase, a liver enzyme that breaks down alcohol safely. I have no idea why there would be sex differences in ADH levels – please let me know if you understand this.)
Here’s what the data tell us about drinking and health:

Risk of death is the lowest (about 80% of the risk of a non-drinker) at about two drinks a week. On the face of it, this suggests people who drink a small amount are much healthier than people who drink nothing at all.
Most researchers are skeptical. Some non-drinkers are alcoholics in recovery (whose bodies have already been damaged by their previous heavy drinking). Others are very sick people who have been warned off alcohol by their doctors. Still others are poor people who can’t afford alcohol. When these unhealthy groups die at increased rates, it looks like teetotaling is bad for you, or like moderate drinking is good for you. The most recent large big study seems to confirm this critique (though see these objections). The CDC currently sides with the skeptics and says that basically any amount of drinking is at least a little bad for you, even if you stay within the recommended guidelines.
But a few people still believe moderate drinking helps, citing for example this review article of randomized controlled trials that showed people randomized to moderate drinking saw improvements on some cardiovascular measures. What I would really like to see are animal studies – whether animals randomized to zero vs. light alcohol consumption had higher mortality. Some people claim these studies have been done and support light drinking, but they don’t provide links and I can’t evaluate them.
Right now I lean to thinking probably there is no protective effect. It’s not obvious what to do with this information. Should we assume healthy teetotalers would do just as well as the current best group, twice a week drinkers? Or extrapolate the line from heavy alcohol consumption backwards and assume they would do better than twice a week drinkers by the same amount that (eg) 30-time-a-week drinkers would do better than 32-time-a-week drinkers?
If we use the first method, we find that men who drink the upper limit of the guidelines have about a 5% higher mortality rate than (extrapolated) teetotalers; if we use the second method, they have more like a 20% higher rate.
Without doing any extrapolation or guesswork at all, just looking at the observed data, we find that men who have two drinks/day more than the limit (ie 4 drinks a day instead of just 2) have about a 10% higher risk of death than the people right at the limit. Bringing back our extrapolations, they also have a 15% – 30% higher risk than (extrapolated) teetotalers.
What does “10% higher risk of death” mean? You can figure it out from this graph (source):

Someone with a 10% higher risk of death will die about one year earlier; someone with a 30% higher risk of death will die about 4 years earlier.
As a very weak rule of thumb, putting these two graphs together, I think it would make sense to say that each extra drink-per-day will take about one additional year off a man’s life, and a little more off a woman’s life. This isn’t quite right, because more accurate graphs show that the trend is exponential – going from your 10th to your 11th drink is worse than going from your 1st to your 2nd – but this only starts making a big difference at very high levels of drinking, and for most people this will be a useful rule.
And it roughly matches results from this study, which finds that people who drink 150 grams of alcohol weekly (a little over one drink a day) live six months shorter than people who drink less than this. People who drink about 300 grams weekly (a little over two drinks a day) live about two years less, and people who drink more than this (a catchall bin anywhere from three drinks/day up) live about five years less.
It also potentially matches this study from Scandinavia which finds that severe alcoholics (people admitted to a hospital with alcohol use disorder) die about 25 years earlier than the general population (ie around age 50), if we assume these people are drinking about 25 drinks per day, which would not be atypical for a severe alcoholic.
Along with increased risk of death, alcoholics are at increased risk for various unpleasant diseases, and tend to look and feel older and be less healthy than non-drinkers of the same age.
2. How can I tell if I’m an alcoholic?
Alcoholism probably isn’t a taxon; there isn’t some hard-and-fast line dividing people into alcoholics and non-alcoholics. There are just people who drink more or less, and who find their drinking is harming them more or less. So only you can answer this question. Are you unhappy with the amount you’re drinking? Do you feel like you can’t stop? Is it reaching a point where it’s harmful to your health, your relationship, or your ability to do the things you want to do? Is it harmful enough that it’s worth using the label “alcoholic” to signal that you feel like things are out of control and you need to start thinking about yourself in a medical way?
In case that answer is too vague to be useful, people have come up with various heuristics that you can use to judge how concerned to be. The most famous is the CAGE questions:
1. Have you ever felt you needed to cut down on drinking?
2. Have people ever annoyed you by criticizing your drinking?
3. Have you ever felt guilty about drinking?
4. Have you ever felt you needed a drink in the morning (“eye-opener”) to steady your nerves or get rid of a hangover?
If you answer “yes” to at least two of the questions, you should at least consider the possibility that you might have a drinking problem. When experts do a more thorough evaluation on people who gave at least two “yes” answers to the questions above, they end up diagnosing on average 77% of them with alcoholism.
Doctors very specifically don’t diagnose alcoholism based on number of drinks per day, because some people are able to drink a lot without having too many problems, and other people start having problems even at seemingly low levels. But if doctors did diagnose alcoholism based on drinks per day, I think the cutoff would be around 4. I’m gathering this from this article saying that about 12% of Americans have an alcohol use disorder, plus this article giving percentiles of alcohol use; the heaviest-drinking 10% of the male population starts at about 4 drinks a day. So if we wanted to come up with a completely number-of-drinks based criterion for alcohol use disorder in men, and keep the same percent of the population alcoholic, it would be around 4. I have known people (especially women) who were definitely alcoholic even though they drank much less than this. I’ve also known people who seem to be doing okay with more – but these people are probably taking five plus years off their lives, so I’m skeptical of their claims that they can “quit any time they want”. Why don’t they want to?
— 2.1. But what is alcoholism, exactly?
This is a good question; instead of me answering it, please accept this IOU for a broader Lorien Psychiatry page on the nature of addiction.
The very short version is that, while free will isn’t exactly an illusion, it’s an abstraction on more complicated calculations that your brain uses to determine what to do at any given time. One input into this calculation is based on whether similar actions have gone well or badly in the past. The brain processes information about how well an action is going using a chemical called dopamine in a structure called the nucleus accumbens; the more dopamine, the more surprisingly well the action has gone and the more you try to do it in the future. Alcohol increases the level of dopamine in this structure. It’s not exactly clear why, but the most likely explanation is something like – it vaguely resembles GABA, an important neurotransmitter which decreases activity in the brain, and it probably decreases activity in some key regulatory structure in a way that lets an abnormal amount of dopamine build up inappropriately. Your brain interprets this as a sign that drinking alcohol has gone very well and it should do it more often.
This is massively oversimplified and leaves out all the complicated psychological and social factors involved in addiction – hence me asking you to accept the IOU.
3.1. I think I’m alcoholic; can I just quit on my own, or do I need medical help?
Studies of people attempting to quit alcohol without treatment find success rates between 21% and 45%, depending on the population and how you define “success” (often something like drinking within the guidelines after a year). Surveys of successfully recovered alcoholics found that 77% recovered without formal treatment.
This doesn’t mean that treatment doesn’t work. It just means that many alcoholics are able to recover on their own. Many others aren’t, and some of these find treatment pushes them over the edge and gives them the help they need to stay sober.
Probably the most practical answer to this question is that it doesn’t matter what I say. Most alcoholics are going to start out feeling like if they just used a little more willpower, they could solve their problems without having to attend any annoying groups or take any annoying drugs. I think it’s fine for them to test this. A few of them will succeed and be very happy. The rest will have learned something important, and gained more resolve for trying tougher options.
3.2. Can I just switch to moderate drinking, or do I have to be completely abstinent?
It’s possible to switch to drinking moderately, and some people are successful at this. But studies consistently show that people who try complete abstinence get better results. And the more severe your alcohol problem, the less likely moderate drinking is to work.
I don’t know of any controlled trials that randomized alcoholics into abstinence vs. controlled drinking groups and saw what happened. All existing research lets the alcoholics themselves decide what to try. Usually more severe alcoholics choose to try abstinence, and less severe alcoholics choose to try moderate drinking. This introduces a potential confounder, though it’s not clear which direction it goes. Since severe alcoholics are tougher cases, maybe it’s even more impressive that the severe-alcoholic-enriched abstinence group outperformed the less-severe moderation group. But also, severe alcoholics might have “hit bottom” and be more motivated to actually try hard. I don’t know, and the research isn’t good enough to tell us.
In this study from Sweden, out of 67 patients in an abstinence-only program, 8 (12%) relapsed to high-risk drinking after two years. Out of 80 patients in a moderate-drinking program, 38 (48%) relapsed during the same time period. Interestingly, somehow some of the people who wanted abstinence-only ended up in the moderate-drinking program, and some of the people who wanted moderate drinking ended up in the abstinence-only program (unclear how, in general they don’t describe their procedures very well). These people failed or succeeded at the same rate as others in their program, regardless of what they came in wanting.
In this study from the US Veterans Health Administration, veterans with alcohol problems used an app called VetChange to work on reducing drinking according to goals they set during the program. After three months, veterans who set a goal of total abstinence had an 84% chance of achieving healthy drinking (ie within guidelines); veterans who set a goal of moderate drinking had only a 25% chance.
This study used results of a large nationwide survey over three years to track how people were doing. In the first year, they identified a group of former alcoholics who were now drinking less than the guidelines. After three years, they reviewed the same survey to see how these same people were doing. People who had been drinking moderately during the first survey were 6x as likely to have relapsed into alcoholism again compared to people who were abstaining.
People with mild cases of alcoholism might be able to get away with moderate drinking (though the evidence suggests that even for this population, abstinence will work at least as well). Harvard Health cites this table from Project MATCH – I think the Alcohol Dependence Scale they’re using is this one:

Trying to switch from problem to moderate drinking doesn’t always just mean saying “Okay, I’ll drink less”. It can require as much work as Alcoholics Anonymous or other abstinence-only groups. See eg Moderation Management (a support group, free) or Moderate Drinking (I think this is a web-based app, hard to tell, $79/3 months). Note that both of these groups suggest you stay abstinent for a month before you start your moderate drinking, in order to “change your relationship with alcohol”. Whether or not you choose to be abstinent long-term, these groups think it’s important to be the sort of person who could be abstinent, and to prove that to yourself.
Some medication strategies constrain you to one of these paths or the other. Antabuse only works with complete abstinence; the Sinclair method of using naltrexone only works with moderate drinking. These drugs have their own pros and cons and you can probably ignore the more generic research if you’re using one of them.
4. Okay, I think I’m alcoholic and I want to quit, what do I do?
If you’re drinking more than about five drinks a day, you may need a plan to withdraw from alcohol safely.
After that, you may want to use a combination of support groups and/or medicine to help you stay off alcohol.
If either the withdrawal or the process of getting medicine or social support feels overwhelming for you, or if you’ve tried doing these things before and they haven’t worked, you might want to go to a specialist or rehab to get more intensive help.
5. How can I safely withdraw from alcohol?
Suddenly withdrawing from alcohol can be dangerous. If you want to quit drinking, you should either taper down very slowly, consult a doctor for help, or go to a hospital/rehab where someone can help you through this.
There is no hard and fast rule about who’s at risk of withdrawal. If you’re at the point where you’re worried you’re an alcoholic and need to stop drinking, you’re probably also at the point where there’s some chance your withdrawal could be dangerous. The HAMS Harm Reduction Network has some predictions about who gets what level of withdrawal how often. Their source is explicitly “we guessed”, but they are a collection of very experienced professionals and former alcoholics, their guesses are probably right, and my guess would have been similar to theirs:

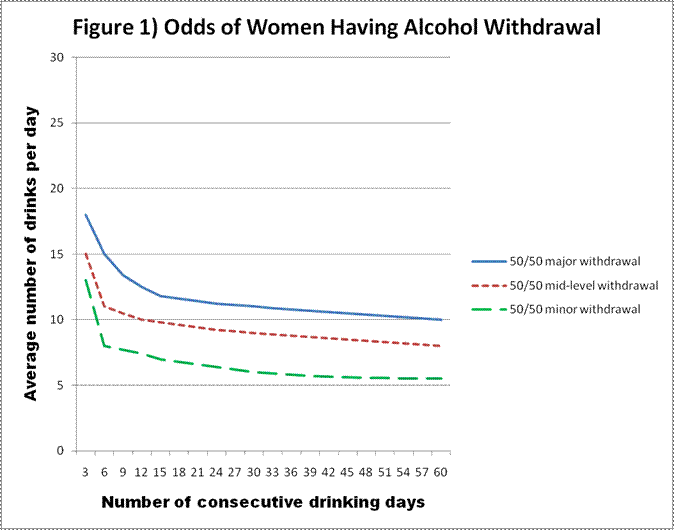
But remember, the lines are where you have a 50-50 chance. You don’t want a 50-50 chance of going into major alcohol withdrawal, or even a 25-75 chance, so you need to be way below the lines. An addictionologist I talked to recounts seeing the odd patient develop severe withdrawal coming off a three drink a day habit. Unless you are drinking a truly miniscule amount of alcohol, there’s no reason not to err on the side of caution and treat the situation as having withdrawal potential.
Alcohol withdrawal can start as early as 6 hours after the last drink, usually peaks around 3-4 days after the last drink, and can last up to a week. Symptoms of minor to moderate alcohol withdrawal are: feeling shaky, feeling anxious, sweating, vomiting, fast heart rate, trouble sleeping. Symptoms of major alcohol withdrawal include those plus confusion/disorientation, hallucinations, seizures, and sometimes death.
If you’re at risk of alcohol withdrawal, you have a few choices.
First, you can try to slowly taper off alcohol at home. HAMS recommends you reduce your drinking at a rate no faster than two drinks per day. So if you’re a 10 drink/day alcoholic, on the first day of your taper, you can drink 8 drinks (evenly spread throughout the day), then the next day 6 drinks, then 4, then 2, then 0. This is a very fast taper and I would go even slower than that, maybe two drinks every few days. The only risk of going arbitrarily slowly is that you might lose motivation and start going back up again before you finish the taper.
Second, you can talk to a doctor. Your primary care doctor should be fine, though if your case is very unusual, you could also seek a psychiatrist or addictionologist. They can guide you through the above process of tapering with alcohol, or they can help by prescribing you an alcohol withdrawal medication you can take at home (usually Ativan, Valium, or Librium). If they give you meds, take them the way your doctor recommends. Usually the plan will be to do a taper over the course of about a week, but using one of these medications instead of alcohol. These are probably slightly better than alcohol to taper with, because they’re “smoother” (instead of having ten drinks at ten different points during the day, you can take Librium once or twice), because they promote sobriety (at least you’re not drinking literal alcohol), and because your doctor controls how many of them you get and will work with you to make sure you take the right amount and don’t cheat. Otherwise there aren’t huge advantages of tapering with these as opposed to tapering with alcohol itself.
Third, you can go to a hospital or rehab for your withdrawal process. They’ll put you on one of the above medications and help guide you as you taper off. This is an expensive option without a lot to recommend it over doing things on your own or with your doctor. The main advantages are psychological – you know you’re being watched by professionals at all times, and you’re in a situation where you can’t succumb to the temptation to pick up a drink. Its main downsides are that it’s potentially expensive (depending on your insurance situation), you’re stuck in a hospital/rehab, and the exact amount of medication you get is the doctors’ decision, not yours. Basically all doctors will manage to keep you from having seizures and dying, but some people who go this route feel like their comfort is not always a top priority. If you go this route, your doctors will probably connect you with resources for managing your future sobriety after you leave the hospital/rehab. Please don’t let rehab’s advertising campaigns make you think they’re indispensible. A good primary care doctor should be able to help you through this for 1% of the cost.
I recommend being very careful about alcohol withdrawal symptoms, and very quick to start worrying about them. You don’t want to let this get to the point where you have the hallucinations and seizures. If you start experiencing anything beyond the very mildest symptoms, either go to the hospital, or drink some alcohol. I cannot stress enough that alcohol treats alcohol withdrawal; a surprising number of people end up in the hospital without realizing this. I sympathize with people who don’t want to have alcohol in the house to tempt them while they’re withdrawing – but if that’s you, have some plan for what to do if you start experiencing withdrawal. A good plan might be to have someone pretty constantly by your side through the week you’re doing this, watching you and ready to take action if things get worse. Going to the hospital is a fine plan, as long as you can afford it and you’re willing to make the 9-1-1 call when the time comes.
6. Is Alcoholics Anonymous a good choice for staying sober?
Some studies show little benefit for any form of support group, therapy, or psychosocial intervention beyond the shortest and most basic. Others find a significant advantage of AA-style support groups over less intensive forms of treatment. Right now the jury is still out. But many individual patients swear by them and say they’ve changed their lives. I’ve worked with some of these people and their stories seem credible. Despite the conflicting evidence, I continue cautiously recommending a support group to people who feel like they need extra help in order to quit.
That support group could be Alcoholics Anonymous, but it doesn’t have to be.
Alcoholics Anonymous itself has some elements of a religious cult. This isn’t necessarily a bad thing! Religious cults are great at pressuring their members to do stuff! Cult leaders are always pressuring people to donate their life savings, or have weird group marriages, or commit suicide – and the pressure often succeeds. Alcoholics Anonymous is an attempt to leverage that same kind of pressure to get its members to quit alcohol. This obviously isn’t the way they talk about it in their brochures, but I think it’s a fair interpretation of their modus operandi. Their cult is generally benevolent, as far as it goes. They don’t demand belief in God (they want “a Higher Power”, but it can be humanity or the Universe or whatever), and they do a good job not pressuring their members into things other than sobriety.
Still, some people really don’t like religious cults, and that’s a valid preference. There are lots of programs that explicitly bill themselves as secular alternatives to AA, including Secular Organizations For Sobriety, LifeRing and SMART Recovery. SOS ditches the God element but otherwise sticks to an AA mindset, where alcoholism is a disease, alcoholics will always be alcoholic, and their only hope is to wage an eternal struggle for sobriety. SMART ditches that stuff too, thinks of drinking as basically voluntary behavior, and is pretty live-and-let-live about people’s choices, including moderate drinking. LifeRing is somewhere in the middle.
A 2018 study tried to compare outcomes across AA vs. AA-alternatives, including LifeRing and SMART. They found that AA was better than some other groups at keeping its members from relapsing into alcoholism, but that the effect was entirely due to AA insisting on total abstinence (which works better), and some other groups allowing moderate drinking (which works worse). People who were in other groups but tried to remain completely abstinent did as well as people in AA.
Most addiction experts recommend what might seem like an excessive frequency of support group meetings: 5-7/week at the beginning, decreasing only after many months if at all. I think the thought process is that if you were previously spending every night drinking, now you should spend every night at your support group, so that you have somewhere to be other than the bar. There’s also a hope that the more completely your support group becomes your entire social life, the more social pressure you’ll face to be sober, and the less you’ll see of your alcoholic (or social drinker) friends. According to AA’s own studies, their average member attends 2.5 meetings/week, but that includes some people who have been there a long time.
7. What medications can help me stay sober?
The best-supported medication for alcoholism is naltrexone (aka “Revia”, “Vivitrol”). This blocks opioid receptors, which changes the way the body processes craving and reward. UpToDate calls it “first-line for most patients”, and addictionologists and patients I talked to praised it highly. If taken as Revia, the standard regimen is 50 mg daily; if taken as Vivitrol, you can get one shot a month. You continue taking naltrexone for as long as you want to stop wanting alcohol; while on the drug, your cravings are significantly reduced. If you spend enough time on naltrexone, your body might naturally stop craving alcohol as much and you can try coming off it. Other commonly used anti-craving drugs include acamprosate (“Campral”) and gabapentin (“Neurontin”), but these (especially gabapentin) have less evidence backing them up. Most primary care doctors know about all of these and will be happy to give you whichever one you prefer.
Disulfiram (“Antabuse”) works differently; it makes you very sick if you drink alcohol. It inhibits acetaldehyde dehydrogenase, the enzyme that helps prevent hangovers. By blocking the enzyme entirely, you ensure that drinking even small amounts of alcohol will near-immediately give you the worst hangover of your life. The target demographic for this drug is people who are committed enough to sobriety that they will take it each morning, but not so committed that they trust themselves not to drink later in the day. It can also work well for people who have a partner willing to watch them take it (I have seen it save a marriage where the wife otherwise didn’t trust that her husband wasn’t going drinking as soon as he left her sight). As long as you take this drug once daily, fear of the inevitable side effects will keep you from drinking. But people who lose resolve and aren’t being monitored can just stop taking the drug and then drink (officially you’re not supposed to take alcohol within two weeks of taking Antabuse, but most alcoholics find they can get away with a little bit after one or two missed doses). Standard dose is a 500 mg/day “loading dose” for two weeks, followed by 250 mg/day thereafter. Antabuse is not a good choice for weak-willed people who will take the drug and then try to drink anyway; this substance is purpose-built to make the experience as painful as possible without actually killing you, consider yourself warned. If you are on this, you have to avoid alcoholic mouth washes, alcoholic lotions (yes! even on your skin!), any fancy dish made with cooking alcohol, etc, etc, etc.

The basic problem of Antabuse: while on the medicine, you will not drink any more alcohol. But you can stop the medicine.
For people who want to try moderate drinking, there’s an alternative way of using naltrexone called the Sinclair method. This exploits naltrexone’s mechanism of action as an opioid blocker: while you’re on it, pleasurable activities don’t trigger your reward circuits normally. Reward circuits’ job is to direct you away from unrewarding activities and towards rewarding ones; if you’re an alcoholic, probably it means your reward circuits find alcohol very rewarding and constantly direct you to it. So the idea is: you take some naltrexone, then drink alcohol. Because your reward circuits are blocked, they register the alcohol as very non-rewarding. They’re a bit confused: they thought this activity was very rewarding, but now they notice it’s not rewarding at all. After doing this enough times, they update their “beliefs” – apparently drinking alcohol is very unrewarding. Instead of directing you towards alcohol, they direct you away from it, towards other activities that are still rewarding.
To use the Sinclair method, you need to religiously take naltrexone an hour before every time you drink (and no other times). If you forget to do this too often, your reward circuits will register alcohol as rewarding, remember that this was the way things were supposed to work, and go back to directing you towards it.
This is less commonly used in the United States compared to some other options (it’s bigger in Europe), but there are online telemedicine providers who will walk you through it and prescribe the naltrexone for you. See eg sinclairmethod.org to connect with some of these people (you will have to be in a qualifying state, but most of the bigger states qualify).
For a generic patient trying to stay abstinent, I would start with naltrexone used normally, plus Antabuse if you think it would help. For a generic patient trying to maintain moderate drinking, I would start with naltrexone used in the Sinclair method.
Some AA-style support groups will look down on you for using medication. This is stupid, and you can probably yourself find a better support group which has successfully joined the 21st century.
— 7.1. Didn’t I hear something about baclofen being a revolutionary new alcohol treatment?
Yeah but it was wrong. See Beraha et al and the Cochrane Collaboration statement.
8. I can’t do this on my own. What are my options for help?
You can start with your doctor. Your primary care doctor can give you a little advice. If they feel out of their depth, you can go to a psychiatrist or an addictionologist (a doctor who specializes in addiction). Your primary care doctor might decide to refer you to one of these people, but if they don’t, you can usually still go on your own, without a referral. Just Google “addiction medicine doctor [your area]” and give them a call.
A step beyond just seeing an addictionologist might be an “intensive outpatient program”. This is different from an inpatient rehab in that in the rehab you live on site, but in the IOP you live at your house and go there during business hours (usually 9-5, five days a week). You probably spend the time attending support groups, seeing therapists and psychiatrists, and learning things about drug abuse and how to prevent it. Your doctor might be able to recommend a good one of these; if not, call your insurance company and see what they think. They might be able to recommend one that’s in network or that their other clients have had good experiences with. If this isn’t covered by insurance, expect it to be expensive, maybe $200 a day for a month.
Rehabs are oversold and of widely varying quality. They don’t have any secret knowledge that an outpatient doctor doesn’t have. Some people find it psychologically helpful to go to a new environment and be away from their usual habits. Other people just want to be somewhere they can’t get drugs (although not all rehabs fulfill even this basic requirement). Consider carefully whether rehab is the best use of your money and energy. If you do decide to go, try to comparison-shop for a good one. Ones affiliated with hospitals are usually trustworthy. Otherwise, consider asking your insurance company – they may be able to tell you which ones are in their network and will be partially covered, or they may just be able to give you helpful advice. If your insurance has no suggestions, look at online reviews, and if you find one you like, ask them if you can come in for a visit. If they say no, that’s a bad sign; if they say yes, see if it looks like a well-run professional empathetic institution. I would be nervous of anything that seems too nakedly capitalist – rehabs that advertise on giant billboards, or try to sell you on expensive aftercare packages before you’ve set foot in their building, or that boast of being “a resort-like environment on the crystal-clear waters of the Caribbean” or anything like that.
(also, for the time being, consider avoiding the entire state of Florida)
9. What are the chances I’ll be able to quit?
Studies on this are very contradictory, probably because it depends a lot on the sample. But about 50% of people who go through alcohol treatment relapse after a few months, and about 50% of people who make it a few months relapse after a few years.
In general, quitting drugs doesn’t work like “you go to a great rehab and then you never drink again”. It looks like a series of slips, some of which are really bad, some of which might even look like going back to heavy drinking for months or years, followed by a series of attempts to quit, some of which are more succesful than others, until gradually they become more and more successful, you spend more and more time sober with fewer and smaller slips each time, and eventually at some point you stay sober forever. While you should always aim to have this be the time you succeed completely and never drink again, you shouldn’t be surprised or discouraged if it isn’t.
One pernicious tendency people have is to spend X amount of time sober, slip, drink a beer or two (or ten), and then say “Well, guess I failed at sobriety, might as well go back to heavy drinking every day”. No, it means you succeeded at sobriety for X amount of time, with only one failure. Pick yourself up and keep going. The people who I see quit successfully are the ones who are able to deal gracefully with occasional failure and continue working hard – not the ones who magically get everything perfect the first time around.
This is a tough line to walk, because if you think you can deal gracefully with failure, that might tempt you to fail. Lots of people will say to act as if the slightest failure will ruin everything. I agree you should act that way, in order to stay motivated. But if you do fail, tell yourself “ha ha, only kidding”, and keep going.
As usual, Piet Hein is helpful here:
The road to wisdom?
Well it’s plain
And easy to express
Err, and err, and err again
But less, and less, and less